Preparing to buy a dental practice may seem like a daunting task. There are many considerations, many of which usually require an expert opinion and guidance. Buying a dental practice involves legal, financing, real estate, and accounting expertise, at the very least, to ensure a smooth deal with the buyer being protected. Here’s what to consider:
Legal
Buying a practice usually means buying the assets of the practice, rather than the corporation itself. In any event, the buyer is taking a significant financial and legal risk and just like any other purchase, you want to make sure that you are getting what you paid for and not any (or at least as little as possible) of the baggage. Every dental transaction should include a well-drafted and thorough purchase agreement which includes substantial representations and warranties by the seller, thorough lists of included and excluded assets, terms addressing restrictive covenants, and disclosures about any potential liabilities affecting the practice. In addition, some transactions might require a portion of the purchase price to be seller financed. In that case, there will be a need for a promissory note and security agreement. As the deal progresses, there might be a need for additional documents to cover an assignment of rights for certain licenses, contracts, and other. Among other things, the final document signed includes a bill a sale, which is like a receipt for the buyer evidencing the sale of the assets.Continue reading

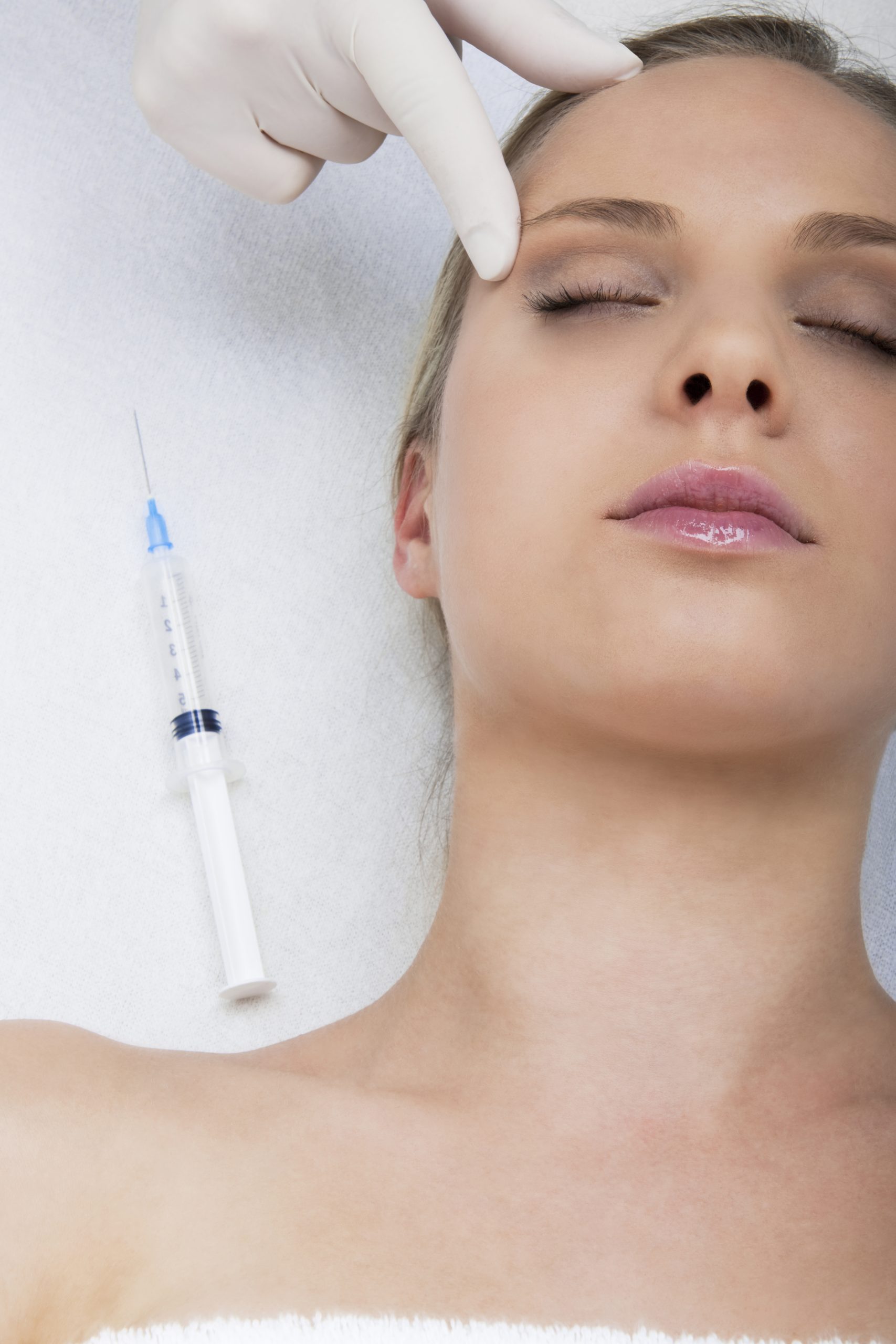
 Medical Spas nationwide, but specifically in Florida, have been opening up at a staggering pace. For many reasons, including new services, technological advances, and lax regulations, the opportunities for
Medical Spas nationwide, but specifically in Florida, have been opening up at a staggering pace. For many reasons, including new services, technological advances, and lax regulations, the opportunities for 
 By:
By: 
 By:
By: 
 By:
By: 
 By:
By: 
 By:
By: