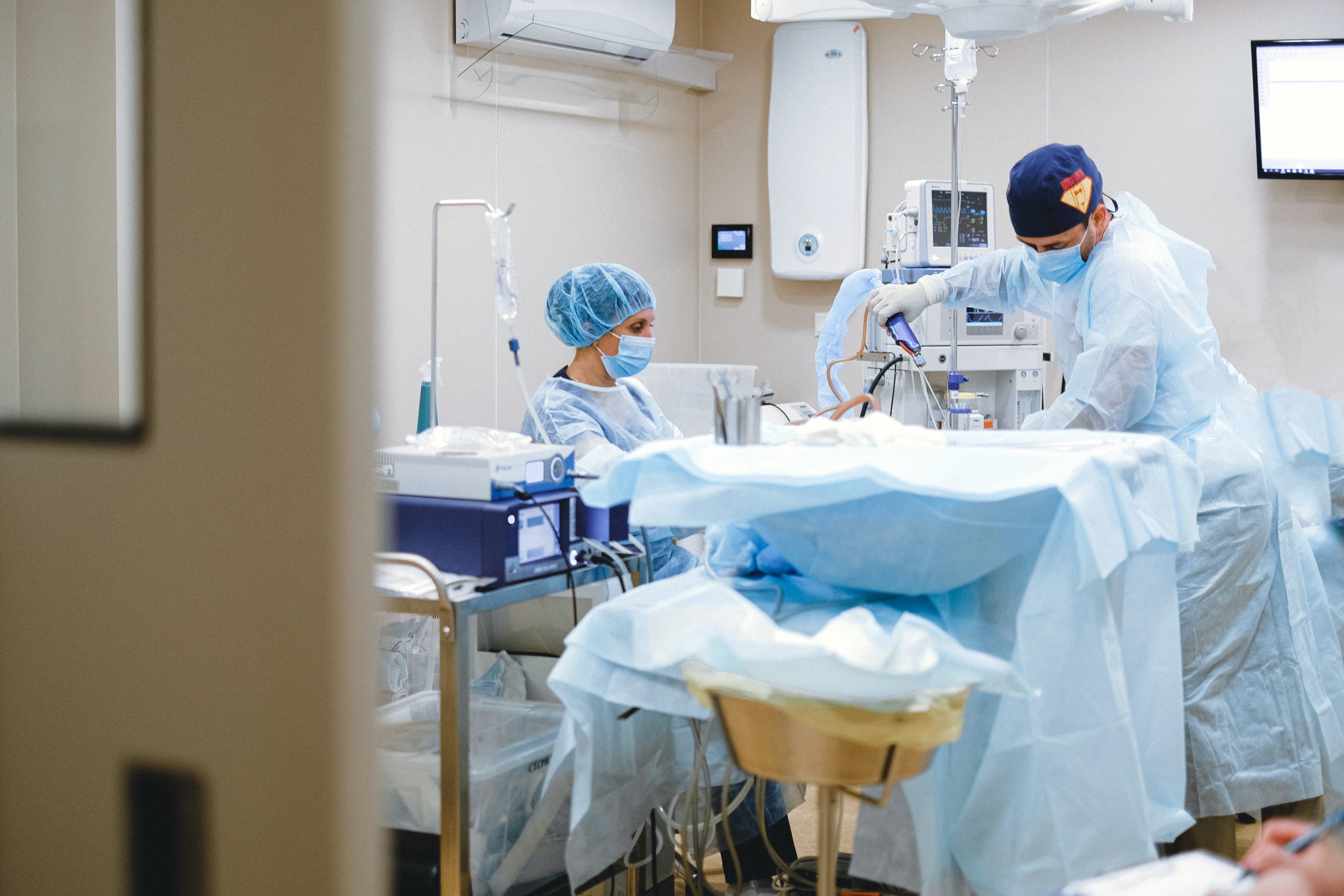
Attorney Dean Viskovich, aka The Lab Guy, gives pointers on what to do when buying or selling a laboratory.
Continue readingThe Debate Over Physician Owned Hospitals
 By: Dave Davidson
By: Dave Davidson
The debate over the pro’s and con’s of physician-owned hospitals has been raging for decades. Physician-owners say their hospitals are more patient-focused, provide higher quality care, obtain better outcomes and therefore receive higher patient satisfaction scores. They also point out their convenience and efficiency.
Opponents argue that physician-ownership leads to overutilization and cherry-picking of only the best patients. The less-desirable patients (both clinically and financially) are then left to be taken care of by the community hospitals. For those reasons, both the American Hospital Association and the Federation of American Hospitals remain strongly opposed to physician-owned hospitals.
Federally, the Stark Law includes an exception which allows a physician to refer patients to a hospital in which the physician has an ownership interest, so long as the ownership interest is in the entire hospital, and not just a subdivision of the hospital. However, in 2010, the federal government weighed in again on the issue, and passed the Affordable Care Act (ACA), which includes provisions which (i) restrict physician referrals to hospitals in which they hold an ownership interest; (ii) restrict any increases in physician-ownership of a hospital; and (iii) restrict expansion of physician-owned hospital facilities. CMS has granted exceptions to these restrictions, but those have been limited to rural hospitals and high Medicaid hospitals, and attempts to amend the law have failed.Continue reading
Webinar | Virtual Practice Workshop: Turning Challenges into Opportunities
 Hosted by Candela and Crystal Clear Digital Marketing, Florida Healthcare Law Firm attorney Chase Howard will be a panelist.
Hosted by Candela and Crystal Clear Digital Marketing, Florida Healthcare Law Firm attorney Chase Howard will be a panelist.April 21 @ 2:00 pm – 4:00 pm
- Download the webinar here.
- Past webinars – free downloads
What’s Missing From Your Physician Employment Contract?
 By: Chase Howard
By: Chase Howard
The average physician employment contract exceeds twenty pages, not including exhibits. While they all include basic terms related to compensation, length and restrictions, many simply do not contemplate important terms that have serious impacts on physician’s daily lives. A physician’s first employment contract is the most significant financial decision of their lifetime. The same can be said for each subsequent contract, which means that understanding, and negotiating, your contract is the most valuable investment you can make prior to entering into a contract.
To understand what’s in your employment contract, simply read it over a few times. To understand not only how those terms affect you, but also what isn’t in your contract, hire an experienced health care lawyer.Continue reading
Physician Engagements: Who Do I Really Work For and Does it Matter?
 By: Randy Goldberg, Co-Counsel
By: Randy Goldberg, Co-Counsel
I am a successful physician who works for a thriving practice that is affiliated with a local hospital or Ambulatory Surgical Center (“ASC”). The hospital/ASC was so impressed with my professionalism and skills that they retained me to perform certain additional duties and services for them. Of course, they are paying me for my time and services. This is great, I love my work, I am generating two sources of respectable income – all is good.
Not so fast!
As can sometimes be the case, all is good while there is smooth sailing and while the money is coming in. However, once there is a bump in the road, a hiccup in a procedure, or a third party employee files a complaint with the Equal Employment Opportunity Commission (“EEOC”); the Florida Commission on Human Relations (“FCHR”); Department of Labor (“DOL”) or any federal or state agency complaining about some alleged incident in their workplace. Their filing of a lawsuit can be against you individually, against your practice or against the hospital/ASC. Not to mention, a lawsuit can be filed by a patient or third party against the practice or the hospital/ASC. Then what?Continue reading
Physician Employment Contracts: Hidden Terms
 By: David Davidson
By: David Davidson
Over the past few years, it seems like physician employment agreements are getting shorter and shorter. While I applaud all efforts towards efficiency and economy, you should not always take those documents at face value. For example, I recently reviewed a one page employment contract for a client. That single page basically said, “We are hiring you as our employee for a term of one year, with an annual salary of $$$.”
At first glance, the simplicity of that document might seem refreshing. That’s especially true if you’re worried about how much time it’s going to take for your lawyer to get through it! My client’s second glance revealed a multitude of unanswered (and essential) questions. There was no mention of expected duties, schedules, standards, renewals, terminations, insurance, benefits, vacation time, sick leave, CME, etc. in the employment contract However, when we reviewed the contract together, we discovered that although those points were not even referenced on that single page, they were still legally, “in there.”Continue reading
Healthcare Trade Secrets: How to Protect Your Practice’s Trade Secrets
 By: Shobha Lizaso
By: Shobha Lizaso
“Prevention is better than cure” is a maxim that has reigned in the healthcare industry for thousands of years; however, this phrase echoes through the halls of the legal profession as well.
Healthcare practices often neglect to appreciate the value of their confidential information as assets and the need to protect these assets. Although HIPAA and HITECH compliance aids in maintaining the confidentiality of patient records, it does not protect a provider’s trade secrets.
Trade secrets of a healthcare practice may include any of the following: patient lists, financial information, contract rates, contract terms client lists, collection rates, marketing tactics, pricing/discount information, and methods of doing business. If leaked, this information may be used by competitors to secure advantages over a healthcare practice. For example, patient lists could be used to solicit a practice’s patients or contract rates and terms can be used by a competitor to undercut the rates of a practice.Continue reading
Physician Compensation Targeted by the Department of Justice
 By: Jeff Cohen
By: Jeff Cohen
The DOJ reported on August 5th a settlement with a South Carolina hospital concerning physician compensation. Though certainly not the first or the biggest case of its kind (e.g. note the Halifax Hospital and North Broward Hospital District cases, which generated settlements of over $100M and $60M respectively), it’s attention grabbing nonetheless.
The SC case was brought by a whistleblower, a neurologist formerly employed by the hospital. The doctor alleged that the seven year employment agreements violated Stark and the Anti Kickback Statute because the compensation was more than what was legally permissible and was also based in part on ancillary services ordered by the employed doctors. Seasoned readers will understand that the concept of “fair market value” (FMV) is at the heart of regulatory compliance and also that compensation surveys of organizations like the Medical Group Management Association (MGMA) are important guides in term of what is/is not FMV. In the SC hospital case, compensation met or exceeded the top 10% of similarly qualified physicians in the area, which is very interestingly noted by the DOJ (because some of the comp levels were still within the MGMA surveys). In other words, the trend here is for the Feds to push back against comp levels on the high end of the FMV spectrum.Continue reading
Physicians: Start Preparing for 2016 Changes in Healthcare
By: Jeff Cohen
Stepping into 2016, physicians and medical practices must continue to be vigilant about the changing landscape in healthcare. Those who adapt quickly and smartly will thrive, while those who don’t will lose. What can they do?
Stabilize
Stability for medical practices requires two things: clear analytics and fixes. Smart medical practices will examine threats outside the practice and within it. As far as external threats go, the key area to focus on is competition. Do you know what competitors are doing and how they’re different than you?
Internal threats are general revealed in the form of (a) employees that need better training and communication, (b) employees that just need to go, and (c) creating a succession plan for the practice. If the practice is top heavy with older physicians, what plan is in place to ensure that “new blood” is brought in? What recruitment strategies are in place? Can the practice go it alone or does it need a recruitment arrangement with a hospital that can demonstrate a community need? How will the older physicians phase out? Is there a plan in the corporate documents to make sure phase out is slow and planned? What do departing physicians get? What about billing and collection? When was the last time that was analyzed? And finally, coding analysis. Is money being left on the table? Far too many practices actually undercode visits and services out of fear of payer audit. Apart from constituting a False Claims Act violation (though regulators are not fast to indict providers who are underpaid), the differential can mean the difference between a good year and a bad one.
Finally, in light of the fact that regulatory and recoupment activity has never been higher, practices would do well to ensure compliance via a self-audit and compliance plan. This is a different animal than a coding audit. This one looks at all contractual relationships to ensure compliance and augments coding compliance. Continue reading
Tuomey Court Has A Lot to Say
By: Jeff Cohen
The Tuomey decision, U.S. Court of Appeals case out of South Carolina, contains important lessons for physicians, especially as it relates to (1) compensation arrangements with hospitals, (2) proper compensation arising in connection with the provision of designated health services (“DHS”), and (3) the advice of counsel defense.
The concept of DHS arises largely in the context of the federal Stark Law, which in pertinent part (1) forbids physicians from owning and referring to providers of DHS (e.g. PT, rehab, diagnostic imaging, home health, DME, clinical laboratory, inpatient and outpatient hospital services), (2) describes how medical practices can provide DHS to their own patients, and (3) forbids even physicians within a practice from allocating DHS profits on the basis of who ordered or referred to them.
The Tuomey case involves a whistleblower action filed against a not for profit hospital system. The original jury in that case decided that the system didn’t violate the False Claims Act, but the appellate court set aside the verdict using facts and testimony that had be excluded from the jury trial, Tuomey Healthcare System was found to have knowingly submitted over 21,000 false claims to Medicare and the government was awarded over $237 Million (most of it in the form of punitive damages). The government (which often advances the plaintiff’s—“relator” case in whistleblower cases) filed a motion for a new trial, which the trial court granted and the appellate court affirmed.
The case involves the following:Continue reading