 By: Dean Viskovich
By: Dean Viskovich
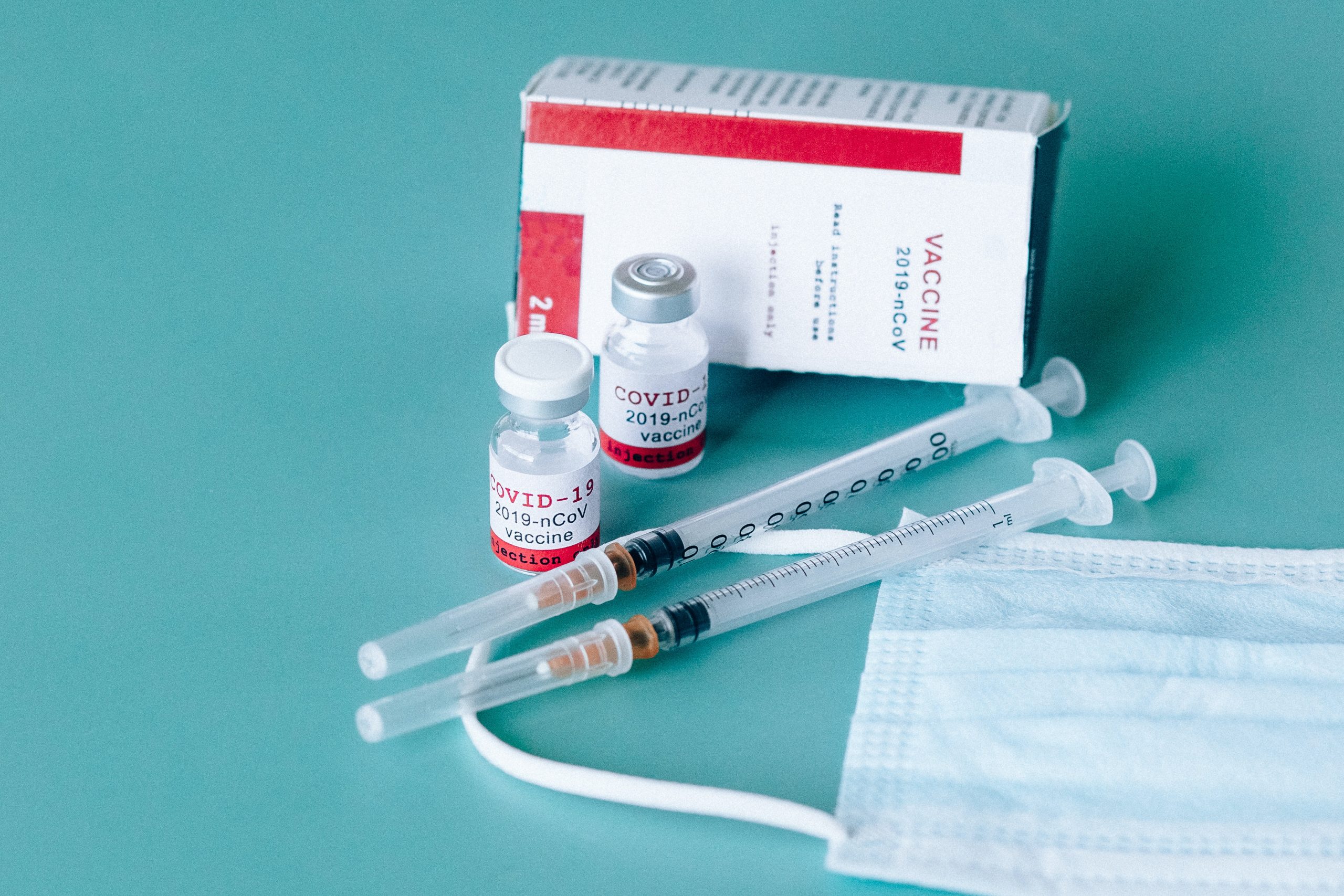
On November 13, 2020 Centers for Medicare and Medicaid Services (CMS) announced that all Americans will have access to the COVID-19 vaccine at no cost. CMS has clearly communicated to private insurers, Medicaid programs and Medicare that it is their responsibility to cover the vaccine at no charge to beneficiaries. CMS states that Operation Warp Speed ensures that States, provider’s and health plans have the information and direction they need to ensure broad vaccine access and coverages for all. As a condition of receiving free COVID-19 vaccines from the federal government, providers will be prohibited from charging consumers for administration of the vaccine.
Beneficiaries with Medicare will not pay anything for the COVID-19 vaccine and their coinsurance/copayment and deductible amounts will be waived. In 2021, for Medicare Advantage beneficiaries, Medicare will pay directly for the vaccine and its administration for those enrolled in MA plans. MA plans are not responsible for reimbursing providers to administer the vaccine. MA beneficiaries do not pay for the vaccine and copayment/coinsurance and deductibles are waived.Continue reading





 By:
By: 
 By:
By: 
 By:
By: 
 By:
By: 
 By:
By: